Dapagliflozin (Synonyms: BMS-512148) |
| Catalog No.GC15530 |
다파글리플로진은 나트륨-글루코스 공동이환체 2 (SGLT2) 억제제로, 신장에서의 글루코스 재흡수를 억제하는 능력에 기반하여 T2DM 치료용으로 승인된 새로운 항당뇨약입니다.
Products are for research use only. Not for human use. We do not sell to patients.
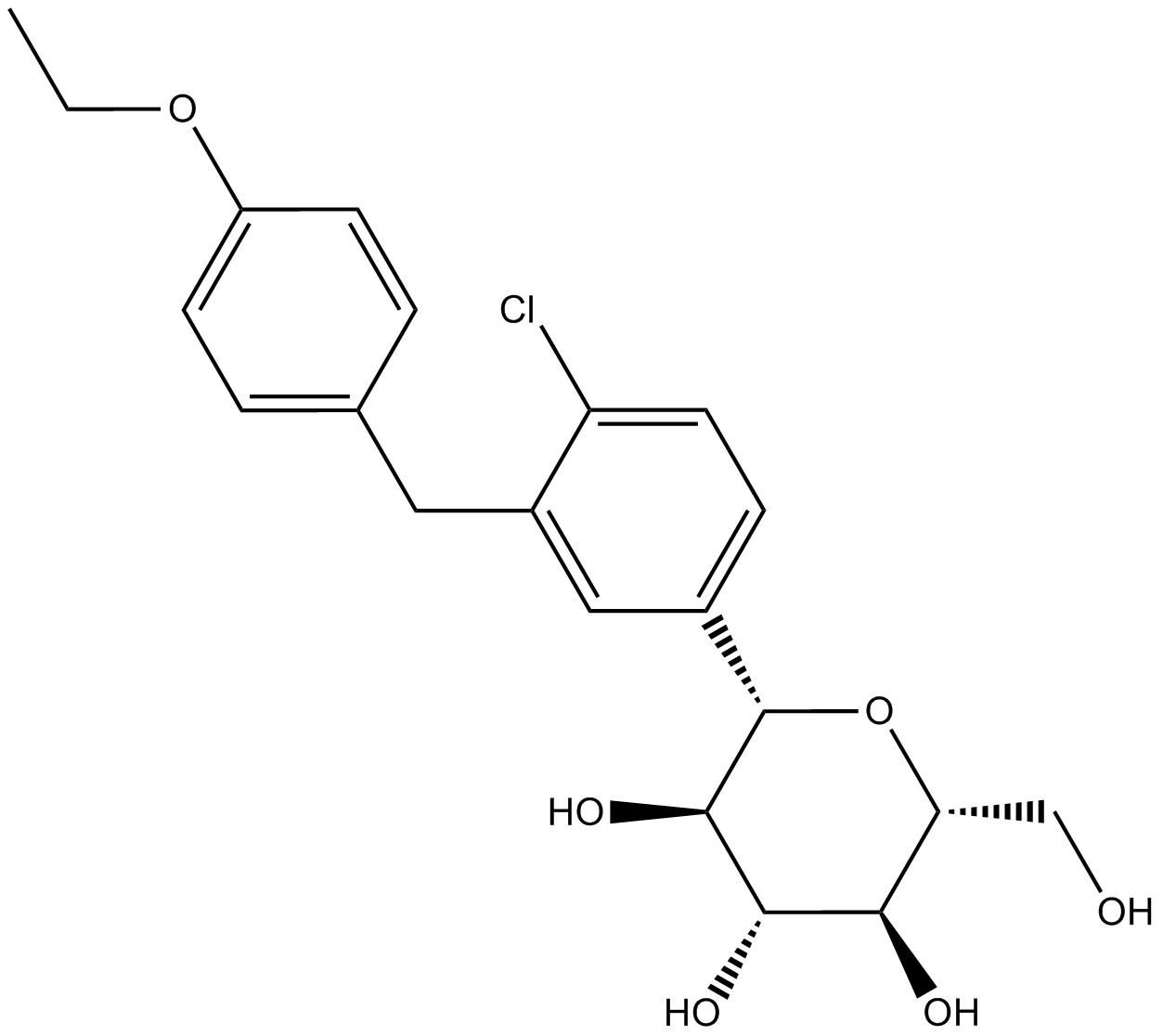
Cas No.: 461432-26-8
Sample solution is provided at 25 µL, 10mM.
Dapagliflozin, a sodium-glucose cotransporter 2 (SGLT2) inhibitor, is a novel antidiabetic agent that is approved for the treatment of T2DM by based on its ability to inhibit SGLT2-mediated renal glucose reabsorption. In addition to providing effective glycaemic control, dapagliflozin help decrease body weight, reduce rate of cardiovascular death, and possibly slow the progression of diabetic kidney diseases[1-3].
Dapagliflozin(20 µM;24h) promoted ACC1 phosphorylation and ACOX1 protein expression, promoted autophagy and alleviated lipid accumulation in PA-stimulated LO2 cells and HepG2 cells[4]. In diabetic proximal renal tubule cells, Dapaglide(20 µM;48h) net improved HG-induced autophagy flux reduction and inhibited mTOR by increasing AMPK activity, meanwhile dapagliflozin inhibited NF-κB pathway inflammatory changes[9].
In db/db mice, treatment with dapagliflozin(1 mg/kg;6 weeks;i.g.) for 6 weeks had little effects on body weight. The fasting blood glucose level significantly declined after the 6-week treatment of dapagliflozin[5]. Dapagliflozin(30mg/kg/day; p.o.) attenuated SGLT2 expression, which could prevent excessive glucose absorption and increase AMPK phosphorylation in HFD-induced obese mice or OA-stimulated HuS-E/2 cells[6]. Dapagliflozin (1mg/kg; i.v.) given pre-ischemia conferred the maximum level of cardioprotection quantified through the decrease in arrhythmia, attenuated infarct size, decreased cardiac apoptosis and improved cardiac mitochondrial function, biogenesis and dynamics, leading to LV function improvement during cardiac I/R injury[7]. Dapagliflozin (1.5 mg/kg;23days; p.o.) provided glomerular protection in mice with protein-overload proteinuria induced by bovine serum albumin (BSA). Dapagliflozin limited proteinuria, glomerular lesions, and podocyte dysfunction and loss[8].
References:
[1]. Dhillon S. Dapagliflozin: A Review in Type 2 Diabetes. Drugs. 2019 Jul;79(10):1135-1146. doi: 10.1007/s40265-019-01148-3. Erratum in: Drugs. 2019 Dec;79(18):2013. PMID: 31236801; PMCID: PMC6879440.
[2]. Plosker GL. Dapagliflozin: a review of its use in type 2 diabetes mellitus. Drugs. 2012 Dec 3;72(17):2289-312. doi: 10.2165/11209910-000000000-00000. PMID: 23170914.
[3]. Plosker GL. Dapagliflozin: a review of its use in patients with type 2 diabetes. Drugs. 2014 Dec;74(18):2191-209. doi: 10.1007/s40265-014-0324-3. PMID: 25389049.
[4]. Li L, Li Q,et,al.Dapagliflozin Alleviates Hepatic Steatosis by Restoring Autophagy via the AMPK-mTOR Pathway. Front Pharmacol. 2021 May 17;12:589273. doi: 10.3389/fphar.2021.589273. PMID: 34093169; PMCID: PMC8176308.
[5]. Wei R, Cui X, et,al. Dapagliflozin promotes beta cell regeneration by inducing pancreatic endocrine cell phenotype conversion in type 2 diabetic mice. Metabolism. 2020 Oct;111:154324. doi: 10.1016/j.metabol.2020.154324. Epub 2020 Jul 23. PMID: 32712220.
[6]. Chiang H, Lee JC, et,al. Delayed intervention with a novel SGLT2 inhibitor NGI001 suppresses diet-induced metabolic dysfunction and non-alcoholic fatty liver disease in mice. Br J Pharmacol. 2020 Jan;177(2):239-253. doi: 10.1111/bph.14859. Epub 2019 Nov 12. PMID: 31497874; PMCID: PMC6989948.
[7]. Lahnwong S, Palee S, et,al. Acute dapagliflozin administration exerts cardioprotective effects in rats with cardiac ischemia/reperfusion injury. Cardiovasc Diabetol. 2020 Jun 15;19(1):91. doi: 10.1186/s12933-020-01066-9. PMID: 32539724; PMCID: PMC7296726.
[8]. Cassis P, Locatelli M, et,al. SGLT2 inhibitor dapagliflozin limits podocyte damage in proteinuric nondiabetic nephropathy. JCI Insight. 2018 Aug 9;3(15):e98720. doi: 10.1172/jci.insight.98720. PMID: 30089717; PMCID: PMC6129124.
[9]. Xu J, Kitada M, et,al. Dapagliflozin Restores Impaired Autophagy and Suppresses Inflammation in High Glucose-Treated HK-2 Cells. Cells. 2021 Jun 10;10(6):1457. doi: 10.3390/cells10061457. PMID: 34200774; PMCID: PMC8230404.
Average Rating: 5 (Based on Reviews and 29 reference(s) in Google Scholar.)
GLPBIO products are for RESEARCH USE ONLY. Please make sure your review or question is research based.
Required fields are marked with *