Mitoquinol |
| Catalog No.GC44205 |
Mitoquinol is a ubiquinone derivative that specifically accumulates in mitochondria due to the covalent attachment of the cation triphenylphosphonium.
Products are for research use only. Not for human use. We do not sell to patients.
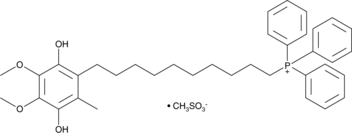
Cas No.: 845959-55-9
Sample solution is provided at 25 µL, 10mM.
Mitoquinol is a ubiquinone derivative that specifically accumulates in mitochondria due to the covalent attachment of the cation triphenylphosphonium. [1 It functions as an antioxidant, preventing lipid peroxidation-induced apoptosis and protecting mitochondria from oxidative damage.[2]
Reference:
[1]. Kelso, G.F., Porteous, C.M., Coulter, C.V., et al. Selective targeting of a redox-active ubiquinone to mitochondria within cells. Antioxidant and antiapoptotic properties. J. Biol. Chem. 276(7), 4588-4596 (2001).
[2]. O'Malley, Y., Fink, B.D., Ross, N.C., et al. Reactive oxygen and targeted antioxidant administration in endothelial cell mitochondria. J. Biol. Chem. 281(52), 39766-39775 (2006).
Average Rating: 5 (Based on Reviews and 39 reference(s) in Google Scholar.)
GLPBIO products are for RESEARCH USE ONLY. Please make sure your review or question is research based.
Required fields are marked with *